Dr Martha Kent was Guest Speaker at the Sanctuary meeting on Tuesday, May 13, 2013.
Dr Kent teaches psychiatrists in BPD.
She also highly recommends Valerie Porr’s book (the one we use): Overcoming Borderline Personality Disorder – A Family Guide for Healing and Change, 2010
Managing the anger
- First, take care of yourself – you have to be there for the long haul
- Use techniques such as therapy, relaxation, sharing the burden, meditation, mindfulness and counselling
- Managing anger starts with managing our own responses. The first temptation for us is to defend ourselves or attack the other person, which is not helpful.
- Know your own emotions, and do not invalidate them. To help you do this, meditate or think about what or how you are feeling.
- The word “dialectic” means “seeking a middle way”. Seek the middle way with your loved one. You need to try to understand what is making her angry right now. Is she for example in some sort of emotional pain?
- Martha recommends the acronym “COAL”: C = Curiosity O = Openness A = Acceptance L = Love
- It’s not right for either of us to allow ourselves to be bullied – if it’s a small issue, ignore it, but if it’s abuse, don’t.
- Do not tolerate abuse. It will not be tolerated by others in the community and neither should we have to. Ignore if possible, but don’t be bullied, rather be respectful of each other.
- Say STOP. Don’t talk to me like that.
- When emotions are high, don’t discuss anything. Soothe and settle first.
- Validate the emotional reaction and check that you have understood how the person is feeling.
- Let some time pass before discussing again. Have a cup of tea, go for a walk, have a bath.
- Try to understand what is going on inside your loved one, that is, what they are feeling and what they are thinking. It is not all about her. We are in the situation as well, and we can model how to deal with anger.
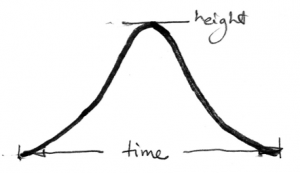
- We need to understand our loved one’s, and our own, “emotional curve” – know how high it goes, as well as how long it lasts – think of it as “emotional temperature”
- Psychiatrists are trained to recognise and pay attention to emotions; Martha recommends you drop what you were doing, pay attention, understand the emotions and validate them.
General comments
- Do not rescue adults from something they can do themselves. It infantilises them. But having said that it is hard to know when to interfere and when to put the responsibility back on them.
- Decide what is your primary focus – if the person with BPD has a child, and you think the child is in danger, the child must be your focus and you must do whatever is necessary to keep him/her safe.
- We have to sit comfortably with the decisions and actions we take.
- The stress on the family is huge, and BPD should be reclassified as one of the most severe mental illnesses, on the same level as schizophrenia
- Marsha Linehan records that DBT groups show significant recovery
- Mary Zanarini’s research is worth reading, but the core of “not wanting to live in their own skin” remains
- Fonagy & Bateman also worth reading on mentalisation – 18 to 24 months treatment gives sustained improvement, lasting for over 8 years
- Winacott refers to the “good enough mother” – says we don’t have to be perfect; even good mothers make mistakes one third of the time
- “Insecure attachment” is common, but might only mean that nobody could have done better; we tried our best, but can’t go back, so we should look at what we can do now with the information we have now.
- Admit mistakes we may have made, acknowledge the mistakes but then say “now as adults, what can we do?”
- Ask “how did I let you down?” Talk in a quiet respectful way. Speak the truth respectfully and calmly.
- We keep looking for the “magic words” that will make a difference, but there aren’t any
Question: Do BPD patients really know how they present?
Answer: Sometimes they don’t eg they might say “I don’t know who I am” or “I wish I’d known that before”
- A BPD person’s moods are extreme, it’s all or nothing
- Inputs from the media tend to exacerbate their perception of self-worth
Labels: Martha is firmly of the opinion that people need to be informed – it works so much better if they know what they have and what can be done about it
Question: Is there a list of “BPD-friendly GPs”?
Answer: No, but maybe that’s something Sanctuary could do
Question: At what age can BPD be diagnosed?
Answer: It used to be 18 and over, but we now know that is not true. Andrew Chanen works with children from the age of 14, and there is increasing evidence that BPD can be distinguished earlier. The Public Mental Health system works against this, but the age boundaries are blurring.
- “pseudo-psychosis” is BPD – usually stress-related.
More posts like this:
Browse our Website by Subject
Main Subjects: Caring for Someone with BPD, Events, Getting Help, Living with BPD, Research, BPD in the Media
Other Subjects: Advocacy, BPD Awareness Week, Couples and Families, Family Connections Course, National BPD Conference, New Member, Sanctuary Meetings, Treatment, Validation, What is BPD
Are you new to all of this? click here
This website is produced by members of the Sanctuary Support Group. We are not mental health professionals nor clinicians. We are ordinary people who care for someone with BPD. This website is a collection of information that we have found helpful or of interest in the context of our own lived experiences. The content of this website is not a substitute for independent professional advice, diagnosis or treatment.
If there is a problem with our website, please contact us here