Dr Martha Kent was Guest Speaker at the Sanctuary meeting on Tuesday, April 11, 2017.
These notes were kindly provided by Liz:
Notes from Dr Martha Kent’s talk
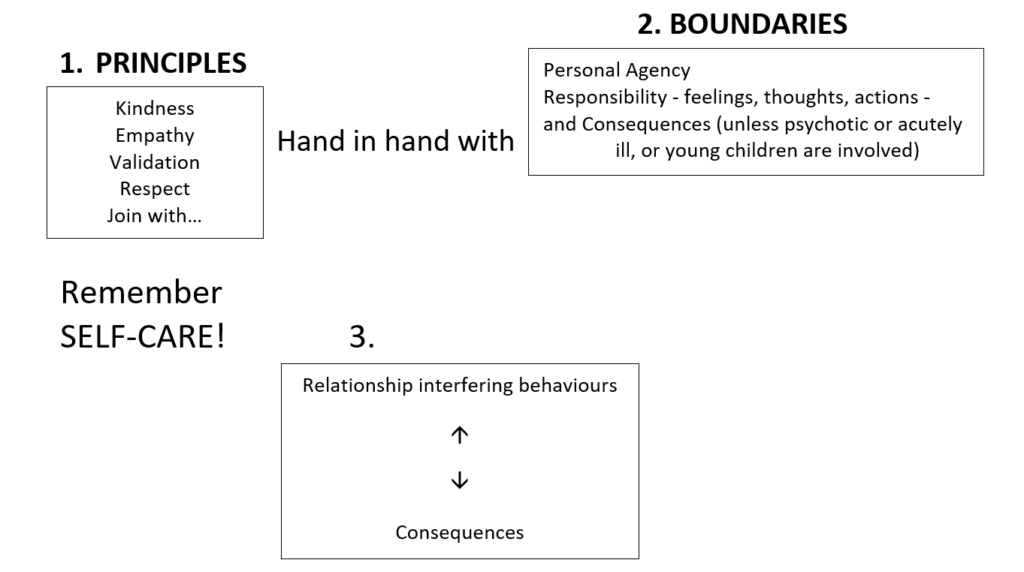
Martha started by explaining her therapeutic framework:
Ask: “Is this my problem?” If not, can’t run with it – would be doomed to fail.
Application of boundaries and notion of responsibility is fraught, but the above principles still apply. As long as the person is not psychotic or acutely ill (e.g. major depression, on drugs, etc), they are responsible for their actions.
No simple answers, much more complex than that.
An important consideration is that we have to live with the decisions we make.
Boundaries – if loved one is abusive, it is not in the best interests of us, our loved one, or our relationship. Abuse is always unacceptable, especially if safety is threatened. It doesn’t fit with a respectful life.
Self-care – think about what you need, and try to meet that. Self-care models good behaviour, and reinforces responsibility for both of you. It is needed for the ongoing wellbeing of you and your relationship with your loved one.
Validation – be careful not to validate dysfunction – don’t reward it. Validate the good stuff. Validation will only take you so far. Remember to validate yourself. Try to be kind. They need to learn to manage their own distress.
Questions
Q: I hear the same thing over and over – how long do I listen?
A: Be honest. Do it kindly. “I know you’re really distressed and I’m exhausted. I can’t do it any more. Why don’t we make a cup of tea and try again another time?” Discuss later, when calm. Set boundaries.
Q: When do I make the boundary?
A: You choose. Encourage calm communication. Depends a lot on the degree of communication – harder to articulate as levels of emotion rise.
Q: When to intervene?
A: Everyone has different breaking points. “That’s terrifying to me. How can I help you?” The person is responsible for telling you what they need.
Too many questions can fall on deaf ears – they may not be able to work it out. “I’m here, if you need me, come and get me”. Or maybe “Do you know what you need? Can be very individual. Lots don’t know. You can ask “What are you feeling?” This creates a pause.
From a carer – Boundary setting can create lots of anxiety for the carer, worrying about what might happen, but it is worth setting a boundary and trying it, and modelling the behaviour that will help both of you. Make them aware of a boundary ahead of a crisis – take time to work out your boundaries.
Q: What happens if she follows me when I leave the house?
A: Ask yourself – Is this my problem? Do what works. Abandonment is an issue – keep this in mind if you leave the room/house. Set limit on how much time you will be away e.g. “I will be back in half an hour”.
There is no particular medication for BPD. Most are on anti-depressants. Medication usually long term. Some/many medications have side effects.
Many people with BPD like to sleep a lot – it is less painful than being awake.
Grief – letting go is important.
BPD – genetic risk is 5 x. It’s not just about trauma, and not just about attachment. Usually a trigger.
? Inheritance of impulsivity, mood disorder, brain problem. All factors play a part. If have some of these factors, BPD is more likely. Hard to say how much genetics plays a part.
Concept of resilience in a BPD environment – it helps if your loved on has people to turn to, is bright/clever, and/or has skills and talents.
Q: Profile of person who is likely to recover?
A: Combination of the above factors. A particular piece of research showed that people who did well were more likely to be upper class, well educated, had stimulating jobs, and certain personal characteristics. Those who had these were very fortunate. Substance abuse increases risk. As one grows and matures, tend to improve.
Classic presentation is “I know I’ve got BPD so I need help”. Often there are co-morbidities e.g. other personality disorders. Narcissistic personality disorder (NPD) diabolical to treat – can sometimes manage the BPD but not the narcissism. People with BPD are attracted to people with NPD. People with NPD can be very controlling.
More posts like this:
Browse our Website by Subject
Main Subjects: Caring for Someone with BPD, Events, Getting Help, Living with BPD, Research, BPD in the Media
Other Subjects: Advocacy, BPD Awareness Week, Couples and Families, Family Connections Course, National BPD Conference, New Member, Sanctuary Meetings, Treatment, Validation, What is BPD
Are you new to all of this? click here
This website is produced by members of the Sanctuary Support Group. We are not mental health professionals nor clinicians. We are ordinary people who care for someone with BPD. This website is a collection of information that we have found helpful or of interest in the context of our own lived experiences. The content of this website is not a substitute for independent professional advice, diagnosis or treatment.
If there is a problem with our website, please contact us here